Peripheral Arterial Disease
PERIPHERAL ARTERIAL DISEASE Q & A
What is Peripheral Arterial Disease?
Peripheral arterial disease, also known as peripheral artery disease (PAD) or peripheral vascular disease (PVD), is a common condition for 20% of Americans, typically aged 65 and older. It can occur in younger patients who have diabetes and other peripheral vascular disease risk factors. It affects the arteries supplying blood from the heart to the farthest parts of the body, particularly the legs.
How Does PAD Develop?
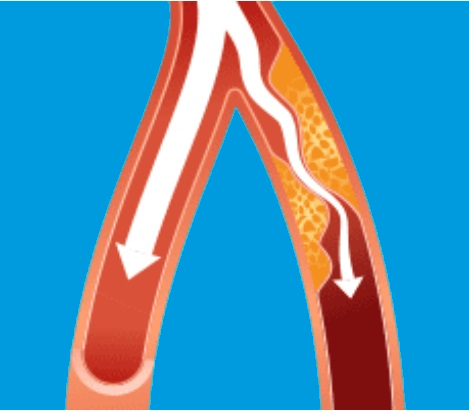
PAD develops because of atherosclerosis, sometimes referred to as hardening of the arteries. This occurs when cholesterol and scar tissue build up, forming a substance called plaque inside the arteries. When fatty deposits of plaque build, arteries can start to narrow or get blocked. Plaque sticks to the artery walls, hardening them and reducing the flow of blood.

Frequently Asked Questions
Peripheral Arterial Disease Patient Education
What Causes Peripheral Arterial Disease?
Plaque that causes PAD can build up for several reasons, including:
- Smoking
- Diabetes
- High blood cholesterol
- High blood pressure
- Obesity
- Having cardiovascular disease
Patients with a history of atherosclerosis in their family are more likely to develop PAD.
Do Patients Need Treatment?
Yes, PAD is a serious condition. Clogged arteries cause decreased blood flow to the legs, which can result in pain when walking. If left untreated, plaque can form clots that block blood flow altogether. This stage of the disease causes critical limb ischemia (CLI) with leg pain that is severe enough to wake patients up at night.
Severe peripheral arterial disease can lead to foot sores or wounds on feet that do not heal. The condition can eventually even lead to gangrene and foot or leg amputation. Gangrene is dead tissue that must be removed quickly, or patients could lose a leg.
PAD can damage tissues and nerves in the legs and increase risk factors for stroke and heart attack. Without treatment, peripheral arterial disease can be fatal.
What Are Symptoms of PAD?
In many cases people do not know they have PAD until they develop complications. Patients are not immediately aware of the condition as it often does not show apparent symptoms.
When symptoms do start, the first is likely to be claudication—pain and cramps in the hips, thighs, or calves when patients walk or climb up stairs. Other PAD symptoms include:
- Coldness in lower limbs
- Leg numbness or weakness
- Leg skin discoloration
- Sores that do not heal
- Slower hair growth or hair loss on legs
- Shiny leg skin
- Slow toenail growth
- Erectile dysfunction
How Is PAD Diagnosed?
An ankle-brachial index (ABI) test is a quick, noninvasive way to predict the severity of peripheral arterial disease. ABI can check how well a patient’s blood is flowing by comparing blood pressure in upper and lower limbs.
ABI uses inflatable cuffs to gauge circulation and measure blood pressure. Systolic blood pressure from both brachial arteries and from both the dorsalis pedis and posterior tibial arteries are measured. The patient must be at rest lying horizontally with face and torso facing up for at least 10 minutes. A handheld 5- or 10-mHz Doppler instrument records the systolic pressures.
Specialized Patient Care
If you have symptoms of PAD or any other leg problems, Dr. Jilbert Eradat can help. With expertise in diagnosing and treating PAD, Dr. Eradat gives each patient individualized attention. Major insurance plans and Medicare accepted.
631 West Avenue Q, Suite A
Palmdale, CA 93551
Phone 661-480-5956
Fax 661-480-5976
Hours
- Monday–Friday
8 am – 5pm
Resources
Connect