Venous Ulcer Treatment
VENOUS ULCER TREATMENT Q & A
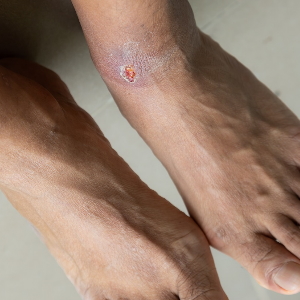
Venous foot and leg ulcers, also known as stasis ulcers, are among the most common types of chronic wounds. It is estimated that up to 1.8 million people in the United States are afflicted with venous leg or foot ulcers.
How Are Venous Ulcers Treated?
A personalized medical treatment plan is best for patients who suffer from venous ulcers. Leg ulcers can be treatment-resistant, sometimes taking months or years to heal.
The first step is compression to relieve pressure in the leg. This may involve wearing compression hosiery, exercising more often, practicing better posture, and prescription medication.
The second step is treatment of the offending vein causing the ulcer. Treating the problem vein will likely produce faster and more complete healing. It also reduces risk of infection, which if severe, can lead to amputation.
Getting fresh, oxygenated, nutrient-rich blood to the site of a venous ulcer helps with the healing process. Treatment involves ablation of the diseased superficial vein and/or treatment of any perforator or tributary veins that lead to the ulcer. This will help re-direct blood flow, alleviate the congestion in blood vessels, and remove any toxins from the area.



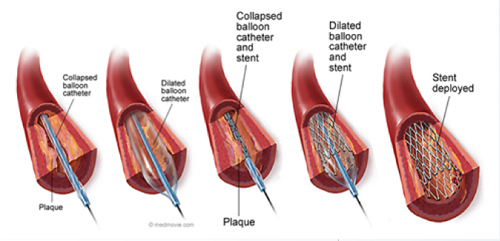
Angioplasty
What Is Angioplasty?
Angioplasty is a minimally invasive procedure to increase blood flow through a blocked or narrow artery. During angioplasty, physicians enlarge the artery’s inner diameter to increase its ability to carry blood to the target. Then, a small balloon usually ranging from 2 to 6 mm in diameter is inflated inside the artery.
How Is Angioplasty Performed?
A small incision the size of a grain of rice is made on the skin overlying the artery. A catheter, or small tube, is inserted into the artery to the point of the blockage or narrowing. A wire is inserted through the catheter which is used to cross the blocked or narrowed part of the artery.
Next, a tiny balloon is placed over the wire and positioned across the blocked or narrowed part of the artery. It is inflated with fluid under x-ray guidance, enlarging the inside diameter of the artery. The balloon is deflated, leaving a channel through the artery’s diseased area, allowing more blood flow to pass.
What Are the Benefits?
Angioplasty increases flow without the need for a complex, painful open surgery. It allows more blood flow into muscles of the leg and foot, relieving pain and allowing more muscle activity while walking, and closing wounds caused by poor circulation.
A hospital stay is usually not required. Most patients return to normal activities shortly after the procedure and major complications are uncommon. Depending on the nature of the lesion, angioplasty may be used in combination with atherectomy and/or stenting to provide longer lasting results.
Atherectomy
What is Atherectomy?
Atherectomy is a minimally invasive procedure which physically removes plaque causing a blockage or narrowing from inside an artery. It is usually performed in conjunction with angioplasty to remodel a blocked or narrowed vessel and allow more blood flow to pass. There are three types of atherectomy:
- Orbital atherectomy – A small burr, like fine grit sandpaper, finely sands down the calcified, hard plaque off the wall of the artery.
- Rotational atherectomy – A small catheter with a spinning blade cuts away plaque and sucks it out of the artery.
- Laser atherectomy – A small catheter that emits high energy light vaporizes blockage inside the artery.
How Is Atherectomy Performed?
Atherectomy is performed during an angiogram procedure, usually in combination with angioplasty. A catheter is inserted into the blood vessel and positioned using X-ray guidance across the blocked or narrowed artery. Depending on the composition, severity, and location of the plaque buildup, an appropriate atherectomy device is selected. Atherectomy is carefully performed until a channel is created or widened in the vessel. Following atherectomy, the vessel is usually widened by inflating a balloon across the narrowing in a procedure called angioplasty.
What Are the Benefits?
Because atherectomy is a minimally invasive procedure, patients usually recover quickly and can return to regular activities faster. Atherectomy allows plaque removal from inside the artery without complex, open surgery. By physically removing plaque build-up, results are often long-lasting and provide a better chance of achieving the desired clinical goal.



Arterial Stenting
What is Arterial Stenting?
Arterial stenting is the act of implanting tiny wire mesh cylinder, known as a stent, within a blood vessel to help keep it open. Stenting is usually performed with angioplasty during an angiogram procedure. Self-expanding metal stents are used to maintain resilient patency and integrity of the blood vessel.
How Is Stenting Performed?
During an angiogram procedure, a small incision is made in the skin overlying the common femoral artery in the groin. A small catheter and wire are advanced to the artery targeted for stenting. After widening the blocked artery or reopening the artery if it was completely blocked, physicians may decide to place a stent or multiple stents. A small tube containing the stent is positioned across the treatment area, and the stent is safely deployed inside the artery. Angioplasty is then performed to fully open the stent. Usually, the patient will be prescribed a blood thinner and aspirin to take at home to prevent blood from clotting within the stent.
What Are the Benefits?
A minimally invasive procedure, arterial stenting does not involve large incisions or stitches and is generally much less painful than open, complex surgeries. Patients benefit from quick recovery and most procedures can be performed on an outpatient basis, without an overnight hospital stay. Medical studies show that arterial stents are more effective than angioplasty alone at restoring long lasting flow through a totally blocked artery, or when the artery is damaged and prone to re-blockage.
What to Expect from Venous Ulcer Treatment?
Dr. Eradat will carefully explain how to prepare for the procedure. He will also provide written instructions. After treatment, the patient’s leg will begin to get fresh, oxygenated, nutrient-rich blood to the site of the venous ulcer, thus helping with the healing process. With the diseased vein collapsed or removed, blood flow in the leg and foot should be more normal, reducing the likelihood of future venous ulcers.
631 West Avenue Q, Suite A
Palmdale, CA 93551
Phone 661-480-5956
Fax 661-480-5976
Hours
- Monday–Friday
8 am – 5pm
Resources
Connect